First call for rabies: Department of Health
The Enterprise — Melissa Hale-Spencer
Joseph Okoniewski, a biologist with the state’s Department of Environmental Conservation, looks at a big brown bat while a red bat lies on his examining table. Homeowners who want to bat-proof their homes, he said, should wait until the young are flying and out. “In the early fall, you can take a lawn chair and sit outside your house at dusk to see where they are exiting.”
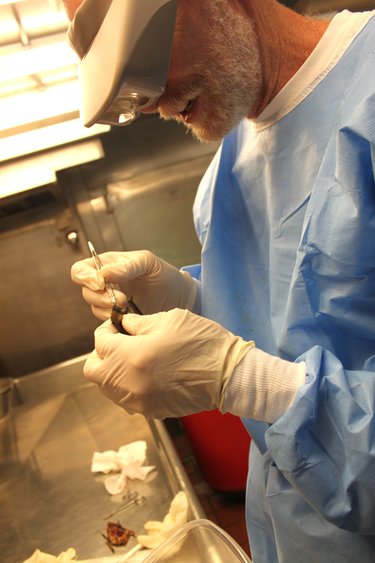
The Enterprise — Melissa Hale-Spencer
Examining a big brown bat suspected of being rabid: Although this bat’s teeth are clearly visible, there have been cases of people contracting rabies from bats where they felt no bite. The Centers for Disease Control and Prevention has said that post-exposure rabies treatment is appropriate even in the absence of a bite or scratch if there is reasonable probability there was contact. This includes a sleeping person waking to find a bat in the room or an adult seeing a bat in a room with a child, a mentally disabled person, or an intoxicated person. This bat, caught by the author, turned out to be rabid.
Enterprise file photo — Melissa Hale-Spencer
Protecting his cattle: The late George Van Etten, shown here in a December 1992 photograph, posed with a pitchfork he used to kill a rabid raccoon before it got into the cow barn on his Knox farm. Raccoon rabies had traveled up the East Coast from the South. The 1993 outbreak of raccoon rabies in New York yielded the highest single-state annual total in the history of the United States with 2,747 laboratory-confirmed rabid animals.
ALBANY COUNTY — About a fifth of all the work done by the county’s health department centers on rabies prevention, estimates Marcia Lenehan, the department’s director.
This involves a staff to answer calls around the clock; nurses to administer shots to people who have been exposed to the disease; outreach with educational materials; and clinics to vaccinate cats, dogs, and ferrets.
“It’s 365 days a year, all those cats and dogs biting,” Lenehan said. “Then, in the spring to the dead of winter, there are the raccoons and bats.”
In the event a person or pet encounters a potentially rabid animal, the exposed person or pet owner should call the Environmental Division of the county’s health department. “Call day or night,” Lenehan said. The daytime number is 447-4620; the nighttime number is 447-4614.
As far as Lenehan knows, “There’s never been a human death in Albany County from rabies, thank God.”
A deadly disease caused by a virus that attacks the brain and spinal cord, rabies came to America in the 1700s when European settlers brought their dogs. In New York State, according to state materials cited by Lenehan, 10 people died of rabies between 1925 to 1944 with all of the deaths linked to domestic dogs. Since compulsory vaccination programs for dogs started after World War II, rabies from dogs was largely controlled by the early 1950s.
There were periodic outbreaks in northern New York from foxes and then, in the 1990s, raccoon rabies that had traveled up the East Coast from the South, arrived in New York. Lenehan, who has been with the county’s health department for 26 years and at the helm since 2007, recalls preparing for the outbreak in the southern part of the county, hosting its first rabies clinic for pets in Berne in the early 1990s.
Then the first rabid raccoon to be identified was “a fluke,” she said, explaining it “hitchhiked in on the back of a truck” and was discovered in Albany near The College of Saint Rose.
The second entered the county as expected, in the Hilltowns. The late George Van Etten, a Knox farmer, killed the rabid raccoon with his pitchfork.
The 1993 outbreak of raccoon rabies in New York yielded the highest single-state annual total in the history of the United States with 2,747 laboratory-confirmed rabid animals.
County literature lists these top six animals as testing positive for rabies in the first decade of this century: over 375 raccoons, over 98 skunks, over 78 bats, over 16 foxes, over 6 cats, and over 5 woodchucks.
Treatment
If a person is exposed to rabies, treatment must begin right away.
The treatment consists of a dose of immune globulin administered as soon as possible after being exposed.
The first five doses of rabies vaccine is given at the same time, with the remaining injections given one each on the third, seventh, and 14th day after the initial injection. The series of shots costs roughly $1,000.
In Albany County, any cost not covered by the patient’s insurance is paid by the county.
Lenehan said that the cost to the county is “actually zero.” She explained, “We have a grant from the state’s health department for $45,000.”
The county’s reimbursed cost in 2013 was $33,000, she said.
“So nobody goes without and there’s no hardship for anyone,” she concluded.
The risk of serious problems for the series of shots is rare, according to the Centers for Disease Control and Prevention. Mild problems are more common. From 30 to 74 percent of patients experience soreness, redness, swelling or itching at the site of the shots, and up to 40 percent experience headache, nausea, abdominal pain, muscle aches, and dizziness, according to the CDC.
Bats
Rabies in bats was first identified in the United States in 1953, and first identified in New York in 1956 with case totals each year ranging from 20 to 84. Bat rabies caused the two most recent rabies deaths in New York — a Sullivan County 11-year-old died in 1993, and a 13-year-old Connecticut resident being treated in a Westchester County hospital died in 1995.
All but two of the 21 human rabies cases acquired in the United States since 1990 have been attributed to bats. Only in two of the 19 fatal cases was there a reported bat bite; another five had some physical contact, leaving 12 with no recognized contact.
The Centers for Disease Control and Prevention has said that post-exposure rabies treatment is appropriate even in the absence of a bite or scratch if there is reasonable probability there was contact. This includes a sleeping person waking to find a bat in the room or an adult seeing a bat in a room with a child, a mentally disabled person, or an intoxicated person.
Lenehan said her department would like to launch a “catch and call” campaign to alert county residents that, if they encounter one of these situations, they should catch the bat and call the department. They should not shoo the bat out a door or window.
She references a short video available at the state health department website that illustrates how to catch a bat.
“It takes just a minute to watch. It shows a girl — a girl,” she said with a laugh. “It looks so simple. It’s not scary at all. My heart would be pounding.”
The basics of catching a bat, as outlined in literature distributed by the county, are this:
— Turn on the lights in the room and close the window;
— Close the room and closet doors;
— Wait for the bat to land;
— Wearing gloves, place a coffee can or pail over the bat;
Slide cardboard under the container to trap the bat;
Holding the cardboard in place over the top of the container, turn it right side up and tape it tightly shut.
The reason it is important to capture the bat is so that it can be tested for rabies. “If a bat is in your house,” said Lenehan, “try to catch it. Call us and we will guide you through it.”
Calls for bats increase with warm weather.
“Bats get more active in August into September,” Lenehan said, “eating flies and bugs to get ready for fall. Once it gets cold, they slow down even more,” she said.
So far this year, according to Mary Rozak in the county executive’s office, two bats have tested positive for rabies in Albany County: One was found in Albany around Academy Road, and the other in a house on the outskirts of Altamont. (This bat was found by the author.)
In 2013, Albany County tested 132 bats and had three positive results; about 2 percent of the tests come back positive, she said.
Pets
People generally know if they are bitten or scratched by a mammal other than a bat.
If a human is bitten by a wild animal, he or she is automatically sent for shots, said Lenehan.
The procedure for pets, largely cats and dogs, varies depending on the circumstances.
According to the state’s public health law, “Animals that have potentially exposed a person to rabies through bite or other means must be evaluated to determine whether they may have been transmitting rabies at the time of the exposure incident….If a domesticated animal remains clinically normal for 10 days following a potential exposure incident, it is assumed that the animal was not shedding rabies at the time of the incident: therefore there was no rabies exposure.”
“Bites to a human from a dog or cat are mostly not rabid,” said Lenehan. “Rabies is rare in cats. The procedure is to watch the cat for 10 days; it will die in three or four days if it has rabies. Watching for 10 days is a standard all over the world.
“If there’s no death, it’s not rabid. If it does die, you test the head to rule out rabies,” said Lenehan, explaining that sometimes pets will die by some other means during those 10 days — say, by getting run over by a car — in which case, they will still be tested.
“If you just want to euthanize right away — we try to tell them to wait 10 days — then they must test….If someone insists, we let them euthanize right away,” she said. “Now you have to cover the cost of decapitating, which is about $60.”
The testing is done at the state’s Wadsworth Center Griffin Laboratory on State Farm Road in Guilderland, she said. Brain tissue samples are examined microscopically, using an immunofluorescence staining technique. The lab does about 9,000 rabies exams annually.
Another frequent circumstance is when a pet encounters a wild animal.
“If an animal is bitten by an animal out in the woods — say a dog and a raccoon have a fight or a dog brings a bat in its mouth back to its owner — if it’s up-to-date on its shots, it just gets a booster,” said Lenehan. “Then you keep an eye on the dog for 90 days and let us know if there is any unusual behavior.”
A dog contracting rabies in a case like that, she said, would be “very, very, very rare; I’ve never seen it and I’ve been here 26 years.”
“If the dog is not up-to-date with its rabies vaccine, you don’t give a booster,” she said. “You watch it for six months. One person has to feed it. It may come down with rabies.”
Lenehan defined several levels of confinement:
—A 90-day observation period, which, as the name implies, involves keeping a close watch on the animal;
— A 10-day confinement period, where the animal has to stay inside and not run free; and
— A quarantine where the animal has to be in a double enclosure, like a cage within a room, or a run within a fenced yard.
An unvaccinated dog that is bitten by a potentially rabid animal must be quarantined.
Sometimes, if there are only adults in a household with no children and few visitors, the county will allow them to keep the dog inside for the quarantine period. Otherwise, a double locked enclosure outside is required. The accommodations are checked by animal control officers.
“It’s awful for the animal and not pleasant for the people,” Lenehan said. “If someone won’t cooperate, they have to pay to quarantine the animal at a vet’s.” She said this happens occasionally.
“Anyone who knows someone who’s been through this gets their pet vaccinated,” she said of the quarantine.
The situations requiring this have declined in recent years, Lenehan said, as the county offers rabies clinics so pets may be vaccinated against rabies.
“Sometimes people are scared so they’re not cooperative,” she said. “They’re afraid we’re going to want to kill their dog…Your pet is safe as long as you follow what we say. Our goal is not to put the animal down.”
Prevention
The simplest and best prevention, said Lenehan, is for people to vaccinate their pets. The law requires pet dogs, cats, and ferrets to be vaccinated by the time they are four months old, again a year later, and then to receive a booster shot every one to three years, depending on the vaccine.
The county regularly holds free clinics.
“We contract with the Guilderland Animal Hospital,” she said. “They provide everything — the vet, the vet tech, the vaccine. We give them all the money we collect.”
The suggested donation is $8 but some give more, she said.
Lenehan also cautions against feeding stray animals, particularly feral cats. “They can harbor rabies and bite,” she said.
The state’s Bureau of Communicable Disease Control recommends disinfecting any surface contaminated with tissues or fluids from an animal suspected of having rabies; using a fresh 10-percent solution of household bleach in water is recommended.
The county recommends bat-proofing homes.
Summer is not a good time to try to bat-proof your house, according to Joseph Okoniewski, a biologist with the state’s Department of Environmental Conservation. The species of bats that have colonies in houses and barns in the summer spend their winters in caves or mines. Homeowners should wait until the young are flying and out, said Okoniewski.
“In the early fall, you can take a lawn chair and sit outside your house at dusk to see where they are exiting,” he said, adding, “You can see droppings at the base of the house.”
And, finally, Lenehan reiterates that, if anyone encounters a bat, is bitten by an animal, or has a pet that is bitten by an animal, the county health department should be called.
“We’re here to help,” she concluded.